Fahim Ahmed Vohra1               BDS, MFDS, MClinDent, MRD RCS
Syed Rashid Habib2Â Â Â Â Â Â Â Â Â Â Â Â Â Â Â Â BDS, FCPS
ABSTRACT: Indirect fixed restorations are a product of multiple clinical and laboratory steps. And at the center of all these procedures is the use of cast and die material and its impact on the definitive fit of the restoration. Dental stone has long been used as a cost-effective cast and die material for fixed prosthodontics. However in cases of periodontally involved teeth having tall and thin tooth preparations, die stones lack the desired ideal mechanical properties of fracture strength and abrasion resistance. Polyurethane resin die material has long been introduced to the dental laboratory technician and has provided a viable alternative to die stone in order to avoid failure in complex prosthodontic procedures. This case report attempts to present the effective use of polyurethane resin dies during full mouth rehabilitation of a patient with generalized tooth wear.
HOW TO CITE: Vohra FA, Habib SR. Use Of Poly-urethane Resin Dies In Prosthodontic Rehabilitation Of A Tooth Wear Case. J Pak Dent Assoc 2014;23(2):80-84.
INTRODUCTION
The fabrication process of an indirect restoration includes multiple clinical and laboratory steps, each of which have the potential to introduce inaccuracies in the definitive restoration. If a dental prosthesis is to be an accurate fit, it needs to be made on an accurate master cast (1-3). According to ISO (International standards organization) die material must comply with certain standards (4), some of which are good dimensional accuracy, accurate detail reproduction, durability and abrasion resistant, thixotropic behavior, ease of manipulation, command set, compatibility with other materials and bio-compatibility (4-7). In conventional prosthodontics a number of materials have been suggested for master cast fabrication. These include die stone, resin reinforced die stone, resins and metal plated dies. Out of those materials that fulfill the requirements of American Dental Association (ADA), type IV dental stone (high strength, low expansion) is almost universally used in dentistry for fabrication of dies and cast in the process of prosthesis fabrication (8).
Reason being, their favorable handling properties, low cost and predictable production of slightly oversized dies when used with elastomeric impression materials. Unfortunately, die stones have poor mechanical properties with low fracture strength and abrasion resistance (6). This means that they can be very easily damaged during complex laboratory procedures. Indeed, it is for these reasons that alternative die materials have been investigated. In order to improve the performance of die stone, resin-reinforced die stones have been developed. However, their surface detail, dimensional stability and hardness were similar to conventional type IV dies stones (6). Copper and silver plated dies have demonstrated exceptional mechanical properties along with good detail reproduction and dimensional stability (9,10). Their routine use may however be precluded by the fact that they are expensive, time consuming to produce and their production is technique sensitive requiring specialist equipment (10). In addition, silver plating is accomplished using a silver cyanide solution, which may produce toxic cyanide gas if mixed with acid. However, in more complex cases involving multiple pick-up impressions their use may be preferred due to superior durability.
Resin die materials are available in the form of epoxy and polyurethane resin. Duke et al,(6) compared transverse strength of different die materials, by three point testing to failure. Die stones had three times less strength as compared to resins. Abrasion resistance of resin dies are shown to be second to metal dies but is greater in comparison to conventional and modified die
stones (6). Resins also demonstrated accurate detail reproduction, recording a line of upto 1 micrometer, whereas dental stone and resin-reinforced stones could only record as low as 17 micrometer (6). Initial reports for dimensional changes of resin dies were unfavorable, revealing shrinkage of 0.09% (6). A recent investigation of contraction levels for epoxy resin using different polymerization methods, reported significant contraction variability, deeming them inaccurate for master cast fabrication (11). Epoxy resin also requires an electric centrifuge to decrease porosity and increase accuracy of master cast. Interestingly, shrinkage for polyurethane resin materials can be controlled by varying silica filler proportions. A polyurethane resin with 60% filler was shown to have transverse strength, which is 2.5 times of dental stone superior to epoxy resin (12). In clinical cases with tall and thin tooth preparations, removal of master cast from elastic impressions most likely result in fractures. Adequately filled polyurethane resin materials, which along with ease of manipulation have increased transverse strength, can perform as an ideal master cast/ die material.
This report will present a clinical case demanding the use of polyurethane resin die material for increased fracture resistance and accurate detail reproduction of multiple tall and thin tooth preparations, in a generalized tooth wear patient.
CASE REPORT
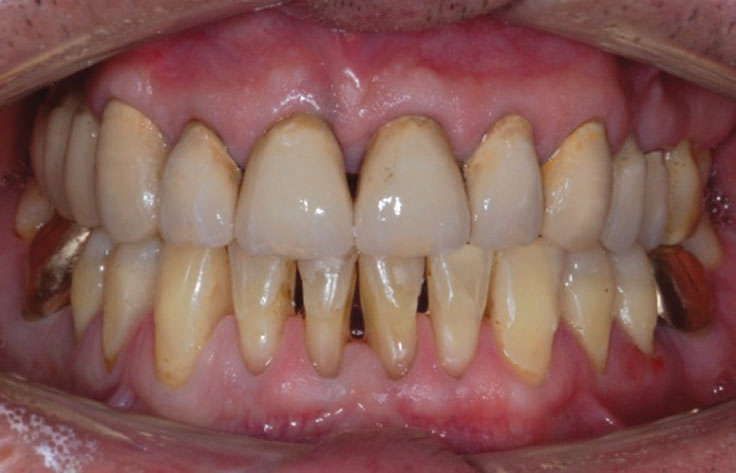
A 57-year-old male patient presented to Edinburgh Dental Institute, Restorative department, with severe maxillary tooth wear and missing maxillary teeth. After complete assessment, which included history, examination, special investigation, articulation and waxup of study casts, the patient was diagnosed to have severe tooth wear in maxilla, moderate tooth wear in mandible (erosion), generalized moderate to severe bone loss in maxilla and mild to moderate bone loss in mandible (from treated periodontal disease) (Fig 1), lack of posterior occlusal stability and missing maxillary right posterior teeth (Fig 2). The definitive treatment plan was executed in the following treatment sequence; (1) Placement of implants at 14 & 16, (2) Gold shell crown (GSC) preparation of teeth 36 & 46 (3) Leveling of the mandibular occlusal plane, (4) Crown preparation

of teeth 13 to 25 (5) Extraction of tooth 24, (6) Provisionalization of complete dentition at the raised OVD (7) Replacement of temporary contact stops with composite, (8) Provision of PFM crowns 13-22, (9) Provision of PFM bridge 23-25, (10) Provision of implant retained PFM bridge 14-16, (11) Provision of gold shell crowns 36 & 46.
After steps 1 to 7 were successfully completed, individual impressions of teeth were recorded after soft tissue displacement using retraction cords impregnated ( Ultrapak, Ultradent Inc, St Louis, USA) with astringent ( Viscostat , Ultradent Inc, St Louis, USA ). Impressions were recorded using dual phase heavy-light technique (Express VPS, 3M ESPE, USA) in PVS material in a stock tray. A decision was made to fabricate individual dies using polyurethane material (AlphaDie MF, Schutz Dental Group, Sylmar, CA,USA) and verify their accuracy by transfer copings. Equal amounts of resin base and filler were mixed in a plastic pot with a wooden spatula and die hardener was added according to
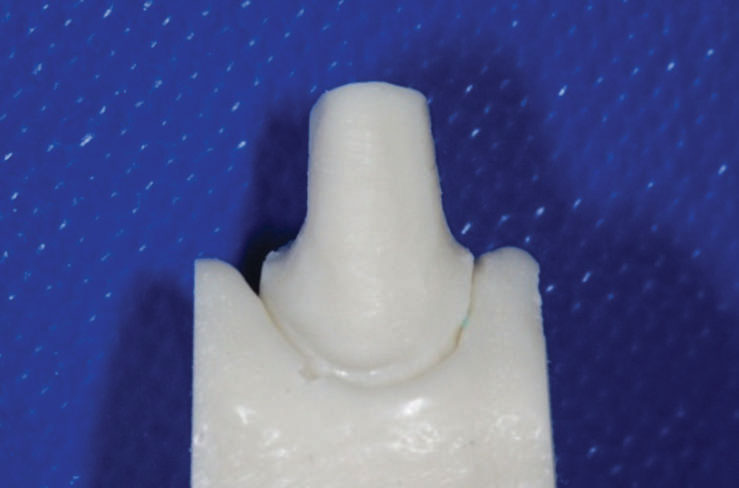
manufacturers instructions to the mix. Pouring of the impression was done on a vibrator within five minutes and complete set was achieved in three to five hours. Individual dies were trimmed and resin (Duralay inlay pattern resin, Reliance Dental Mfg corp, Worth Il, USA) pick copings were fabricated on each die (fig 3 & 4). A


pick up master impression was recorded after splinting the individually seated transfer impression copings in PVS material using a dual phase heavy light consistency technique (fig 5). Registration in RAP was recorded using wax (Alminax Rite Bite, Swindon, UK) and ZOE (TempBond, Kerr, CA,USA). Crowns (13-22) and bridge (23-25) were cemented using a resin based luting cement to enhance retention of the restorations.
Cement retained implant fixed partial denture (14- 16) and GSC’s were cemented to complete the case. The
patient was pleased with the outcome (fig 6) and was reviewed at 3, 6, 12 months, followed by a yearly review for maintenance.
DISCUSSION
Patient was delighted with the outcome of the treatment of his severely worn teeth and was pleased with the fixed replacement of the missing maxillary teeth. Attention to detail at each stage was crucial to the treatment provision and the successful outcome. Patient expectations were identified in the beginning and considered in all treatment decisions13. A diagnostic wax up was completed at the start of the treatment and a mock up in the mouth was performed to allow the patient to assess the proposed treatment results. A reorganized approach was used for rehabilitation of the patient, as space lost due to tooth wear was gained by increasing the VDO14,15.
The prepared maxillary teeth had moderate to severe bone loss from previous periodontal disease16. Firstly, this rendered preparations to be tall and narrow as margins had to be placed equi-gingival for the purpose of aesthetic and maintenance. Preparations were kept conservative, using putty indices from the diagnostic wax up17 and immediate dentine sealing was done18. In order to avoid fracture of dies, resin instead of die stone was used12. Secondly, periodontal tissues were highly susceptible to breakdown due to further disease and trauma from
prosthodontic procedures; hence a complete mouth pickup impression using splinted customized copings was used19. This allowed for minimal trauma as prolong and repeated soft tissue retraction was avoided and aided prosthesis fabrication as soft tissues were recorded in rest state. Lastly, possible tooth mobility of the periodontally involved teeth was prevented by splinting resin copings in the pick-up master impression. Impressions were verified by making individual resin dies, these were in turn verified in the mouth-using pick up copings prior to impression making.
The choice for die material was between metal platted and resin dies, as resin reinforced stone dies have shown mechanical properties almost similar to type IV stone dies6. Metal plated dies are dimensionally accurate, have smooth surfaces and are durable with high strength and abrasion resistance9,20. However unavailability of special electroplating bath and biological hazard of the materials involved prevented their use. Resins provide excellent surface detail, good abrasion resistance, adequate transverse strength (2.5 times of type IV stone)12. In contrast to epoxy resin, impressions can be accurately poured without requiring a centrifuge with polyurethane resin. The suggested shrinkage for resin (Alpha Die MF) by the manufacturer is 0.06% (low shrinkage), this change however was compensated by increasing the filler particles of the mix to 60%12. Handling of the polyurethane resin was challenging, as the properties of the material are highly sensitive to manipulation technique. The material is tacky and sticks to instruments (disposable instruments were used) and has low thixotropy as a result pouring was carried out on maximum vibrations to avoid porosities.
All efforts were made to maintain healthy soft tissue during the provisional phase, which provided an opportunity for assessment of aesthetics and occlusion. Patient was informed that maintenance of good plaque control and excellent OH was essential for the good prognosis of the treatment.
CONCLUSION
In summary, this case report displays the use of polyurethane resin as a viable alternative to die stone for master cast and die fabrication in complex prosthodontic cases, for enhancing the quality of definitive restorations and ensuring successful clinical outcome.
REFERENCES
- Vigolo P, Millstein PL:Evaluation of master cast techniques for multiple abutment implant prostheses. Int J Oral Maxillofac Implants 1993; 8:439-446
- Dilts WE, Podshadley AG, Sawyer HF, et al: Accuracy of four removable die techniques. J Prosthet Dent 1971; 83:1081-1085
- MyersM, Hembree JHJr :Relative accuracy of four removable die systems. J Prosthet Dent 1982; 48:163165
- Anusavice KJ: Phillip’s Science of Dental Materials (ed10). Philadelphia, PA, Saunders, 1996, p. 186
- Brabant A, Grimonster J, Deschamps R,VanBiervlietL. Comparative study of four physical properties of 13 dental stones, “hard†and “extra hard†[in French] Cah Prothbse 1980; 32:145-157.
- Duke P, Moore BK, Haug SP, Andres CJ. Study of the physical properties of type IV gypsum, resincontaining, and epoxy die materials. J Prosthet Dent 2000 ;83: 466- 473.
- Bailey JH, Donovan TE, Preston JD. The dimensional accuracy of im- proved dental stone, silverplated, and epoxy resin die materials. J Prosthet Dent 1988;59:307310.
- AmericanNationalStandardsInstitute/AmericanDental Association: Specification No. 25 for Dental Gypsum products, 2000
- Toreskog S, Phillips RW, Schnell RJ. Properties of die materials: A comparative study. J. Prosthet Dent. 1966;16:119-131.
- Cassimaty EM, Walton TR: Effect of three variables on the accuracy and variability of electroplated copper dies. Int J Prosthodont 1996;9:547-554.
- Prisco R, Cozzolino G, Vigolo P. Dimensional accuracy of an epoxy die material using different polymerization methods. J Prosthodont. 2009;18:156-161.
- Derrien G, Sturtz G. Comparison of transverse strength and dimensional variations between die stone, die epoxy resin, and die polyurethane resin. J Prosthet Dent. 1995;74:569-574.
- Ibbetson R. Tooth surface loss. 9. Treatment planning. Br Dent J. 1999; 186:552-558.
- Dyer K, Ibbetson R, Grey N. A question of space: options for the restorative management of worn teeth. Dent Update 2001; 28:118-123.
- Davies SJ, Gray RM, Whitehead SA. Good occlusalpractice in advanced restorative dentistry. Br Dent J. 2001;191:421-434.
- Nyman S, Lindhe J. A longitudinal study of combinedperiodontal and prosthetic treatment of patients with advanced periodontal disease. J Periodontol. 1979; 50:163-169.
- Magne P, Belser UC. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J Esthet Restor Dent. 2004; 16:7-16.
- Magne P. Immediate dentin sealing: a fundamentalprocedure for indirect bonded restorations. J Esthet Restor Dent. 2005;17:144-154
- Wallace FH. Resin transfer copings. J Prosthet Dent1957;8:289-292
- Fan PL, Powers JM, Reid BC. Surface mechanicalproperties of stone, resin, and metal dies. J Am Dent Assoc. 1981;103:408-411
- Assistant Professor, Prosthetic Dental Science Department. Address: SDS, College Of Dentistry, King Saud University
- Assistant Professor, Prosthetic Dental Science Department.College Of Dentistry, King Saud University.
Corresponding author: “Dr. Fahim Ahmed Vohra†< fahimvohra@yahoo.com >